Blogs
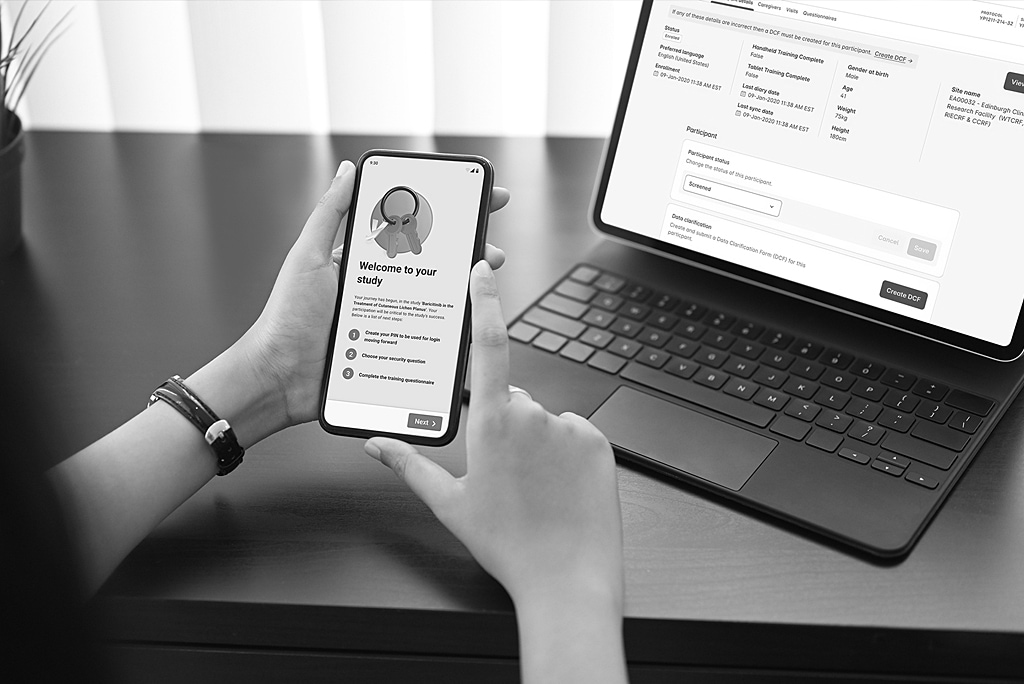
GLP-1 Clinical Trials and Connected Devices: Ensuring Data Excellence with Precision Technology
Learn how connected devices and eCOA platforms in GLP-1 clinical trials boost data quality, reduce errors, and accelerate trial success…
What the ICH E6(R3) Guidelines Mean for IRT Companies Today
Learn how IRT/RTSM providers can align with the evolving GCP landscape…
Gratitude, Grief, and the Call for Continued T1D Research During Mental Health Awareness Month
Kristy Birchard, who has lived with Type 1 Diabetes for over 30 years, shares a personal reflection on the emotional toll of T1D and the…
Accelerating Pain Management Trials: How Advanced eCOA Solutions Reduce Timelines
Learn how eCOA solutions for pain management trials improve data, cut timelines, and enhance trial efficiency…
GLP-1 Clinical Trials: Opportunity for Innovation
Discover how YPrime supports GLP-1 trial innovation through advanced eCOA technology…
Busting the Myths: Clinical Trial Translation and eCOA Instrument Licensing
Are your global trials being held back by misunderstandings about translation and licensing? Clinical trial translation and licensing…
Speaking the Language of Inclusion: Localization’s Role in Giving a Voice to All in Clinical Trials
Localization is more than just translation—it’s about breaking down language barriers to ensure clinical trials are truly inclusive…
Building Better eCOA: Quality, Engagement, and Scientific Integrity
Explore how YPrime’s patient-focused approach to eCOA enhances data quality, boosts patient engagement, and drives scientific excellence…
GLP-1 Clinical Trials: 5 Key Strategies and 5 Pitfalls to Avoid
Success in GLP-1 clinical trials requires a balanced approach that combines innovative strategies with careful attention to potential pitfalls…
We’ve got you covered with strategies and solutions to improve your clinical trial technology, reduce clinical research site burden, and transform your patient experience.
Let’s get started today!